
Artificial intelligence in insurance claims has moved beyond experimentation and is now the single most important test case for operational transformation.
In-depth interviews with 35 non-life insurers, consloidated within the Sollers AI Report, highlight that adoption of AI in claims is widespread and a focal point of investment for automation:
- 66% automate document and email extraction in claims
- 57% deploy chatbots in claims journeys
- 82% use or are implementing large language models
- 85% expect AI to have a significant to disruptive impact on claims handling efficiency in the next 3 to 5 years
Recent AI advancements enable better data structuring and automation of end-to-end activities leading to a more robust and efficient claims handling process.
Discipline in the adoption of AI within claims will determine which insurers convert AI from a technology initiative into a structural cost and risk advantage.
Intelligent Document Processing
Intelligent Document Processing (IDP) and data extraction emerge as critical enablers within the automation of claim handler activities. They are rapidly becoming a commodity as the tools specialised in document processing are already highly developed with comprehensive IDP platforms and a range of dedicated AI models offered by major cloud providers.
Full automation requires the extraction of data from documents across 5 steps: triaging incoming mails, separating combined documents, deduplication, classification and data extraction.
However, a high degree of automated intelligent document recognition and data extraction does not necessarily result in a fully touchless claims handing process.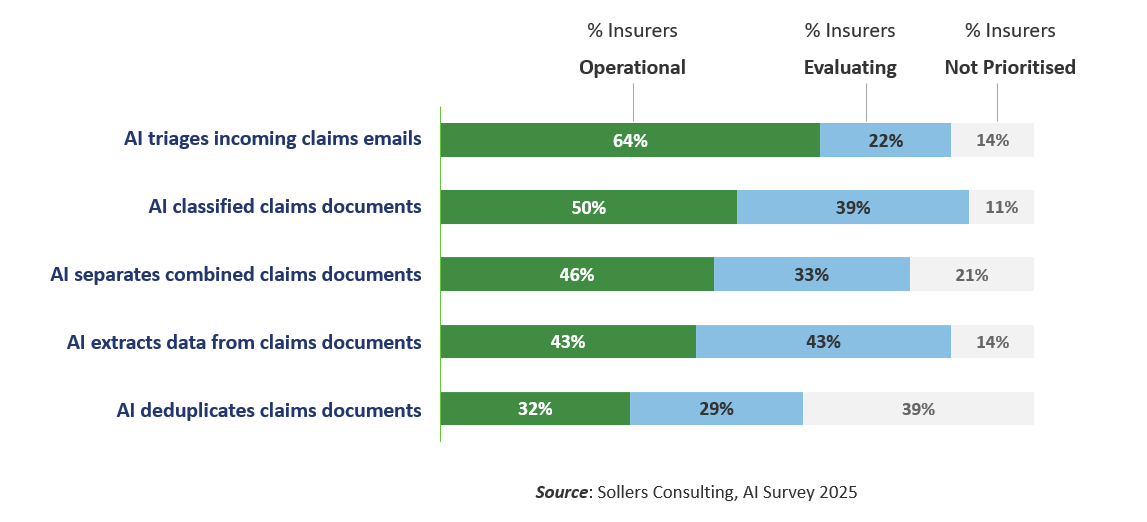 Figure 1 - AI Support for Processing Documents and Emails in Car Insurance Claims
Figure 1 - AI Support for Processing Documents and Emails in Car Insurance Claims
AI-Powered Chatbots
Within automative insurance claims the use of AI chatbots to answer generic claims questions is relatively common (~42% of insurers), however, their use for answering more specific claims questions, supporting FNOL (First Notice of Loss) or making claim updates have a relatively low adoption (23%, 8% and 8% utilisation respectively).
Not all insurer business models require a chatbot channel, but integrating sophisticated natural language AI solutions into end-to-end claims processes is often costly because of legacy systems and siloed data architectures. This can make the required level of investment relatively high compared to other available solution options.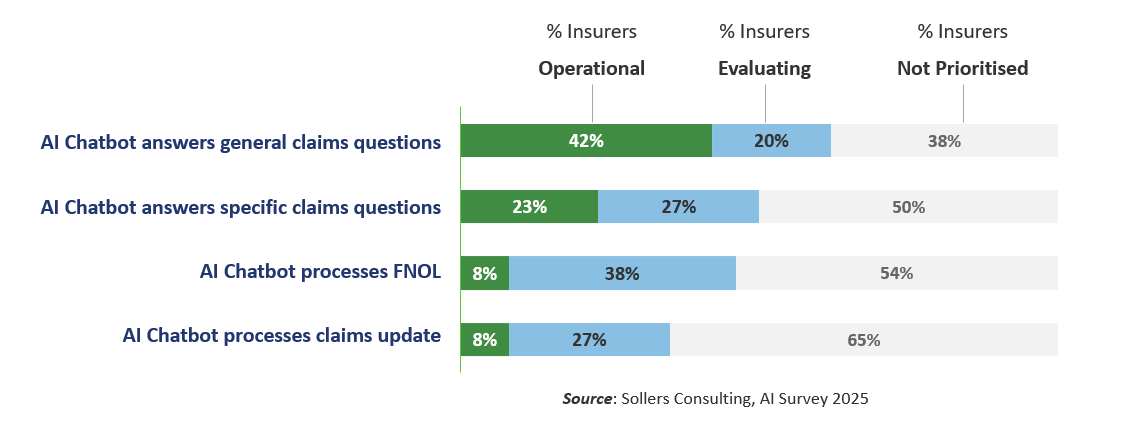 Figure 2 - Chatbot Support in Handling Automative Claims
Figure 2 - Chatbot Support in Handling Automative Claims
Inspection Automation
Inspections are a key step in the claims handling process and most popularly used in automative claims that are characterised by more standardised and volume-intensive inspection processes.
Within car damage inspection, the complexity of the task and the data required for automating the preparation of inspection reports necessitate specialised AI solutions. This is particularly important, as it directly impacts the accuracy of financial payouts. Insurers are gradually developing full automation, thereby minimising the associated risks.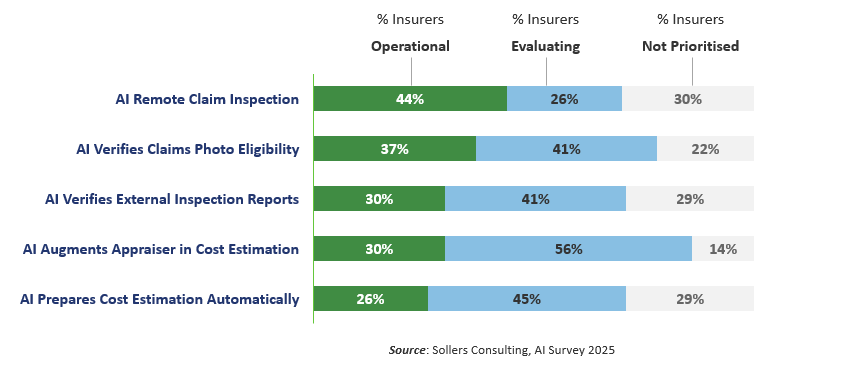 Figure 3 - Automating Inspections in Automative Claim Handling
Figure 3 - Automating Inspections in Automative Claim Handling
Funds Payout
One critical aspect is often overlooked: the final payout of funds. At this stage, business owners need assurance that AI has not made a mistake. Such a mistake could lead to either an overpayment to the client (resulting in financial losses for the insurer) or the denial of a rightful claim. Both scenarios pose a risk of reputational damage for the insurer.
Some AI tools come with built-in confidence level KPIs that can be used to filter out wrong AI recognitions to address this issue, while for others, architects must define their own logic to ensure accuracy.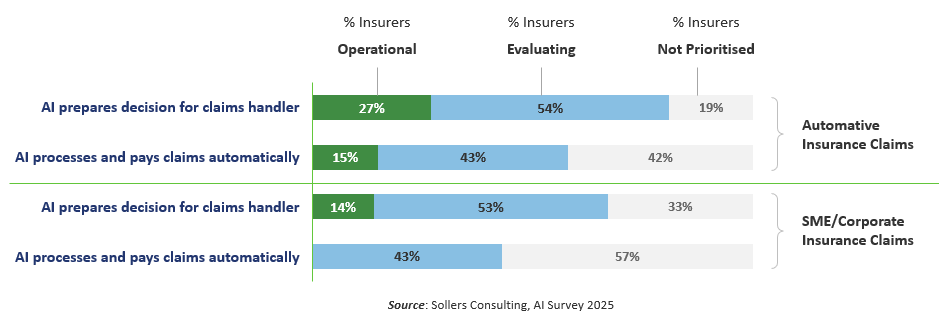 Figure 4 - AI Support for Claim Handlers
Figure 4 - AI Support for Claim Handlers
The Journey to Touchless Claims
Claims handling is a complex process. Transformation typically requires a gradual, step-by-step approach with a broader business shift. Insurers can benefit significantly from automating selected processes.
The automation journey should factor in time and iterative loops for the insurer to learn gradually how to control AI while managing the risk. Automating claims decision making at scale will require the ability to:
- Control correctness of AI outcomes (AI predictions)
- Define and transform architecture (legacy and new components)
- Integrate new and old processes with legacy core claims platforms
- Manage complexity of documents, data, business logic and human-in-the-loop workflows
- Manage compliance of cloud solutions
These capabilities are not uniformly in place and as a result insurers are following a staged path to investing in claims automation:
- Automating document processing
- Enhancing sales systems and processes to capture policy data in a structured form
- Integrating external data sources
- Automating inspections and fraud detection
- Adapting legacy system architecture for real-time processing
- Redefining legacy business processes and customer interactions
The winners will not be those that pursue “touchless claims” as a tagline, but those that are driven by discipline to deliver the optimal outcomes for customers and the business.
Sollers is a global consultancy focused on supporting insurers become future ready through technology. We modernise core claims platforms, integrate vendors and data across complex ecosystems and optimise end-to-end claims performance.
SOLLERS AI REPORT
Beneath the Surface of AI in Insurance:
Insight-Led, Experience-Driven
SOLLERS AI REPORT
Beneath the Surface of AI in Insurance:
Insight-Led, Experience-Driven
Authors of the article
 Charles Whatling - Head of General Insurance
Charles Whatling - Head of General Insurance
 Piotr Kondratowicz - Business Architect
Piotr Kondratowicz - Business Architect
Technology & Market Insights




CEO Voices
CEO Voices – Interview with Andrej Slapar, President of the Management Board of Zav...

